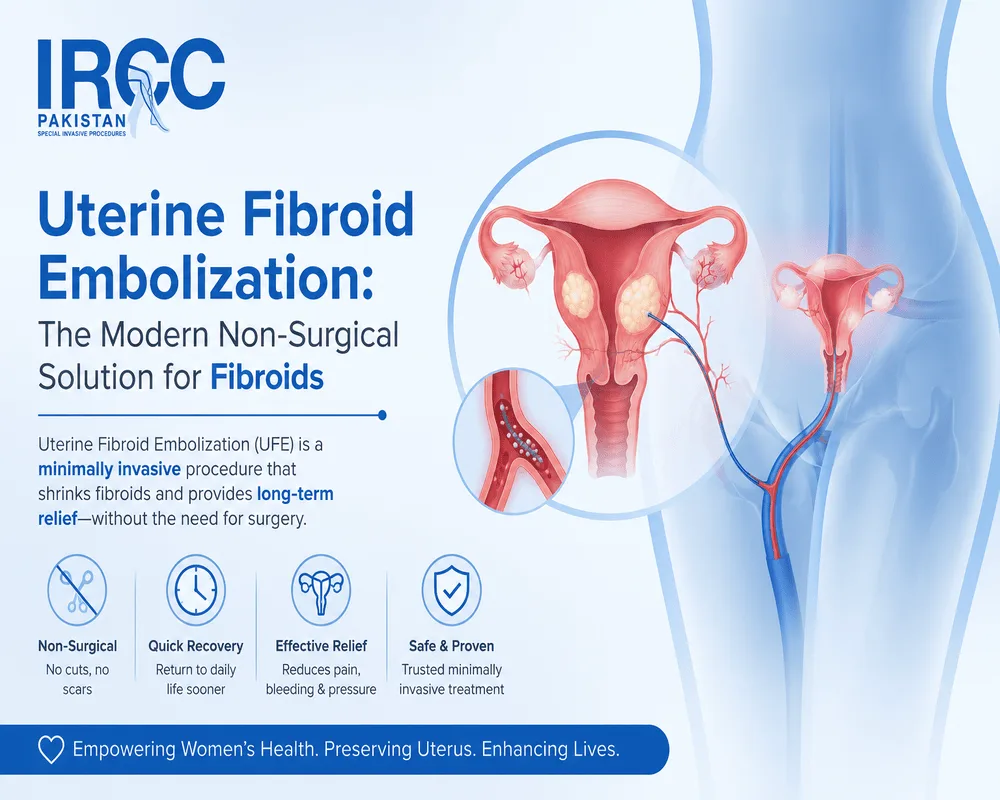
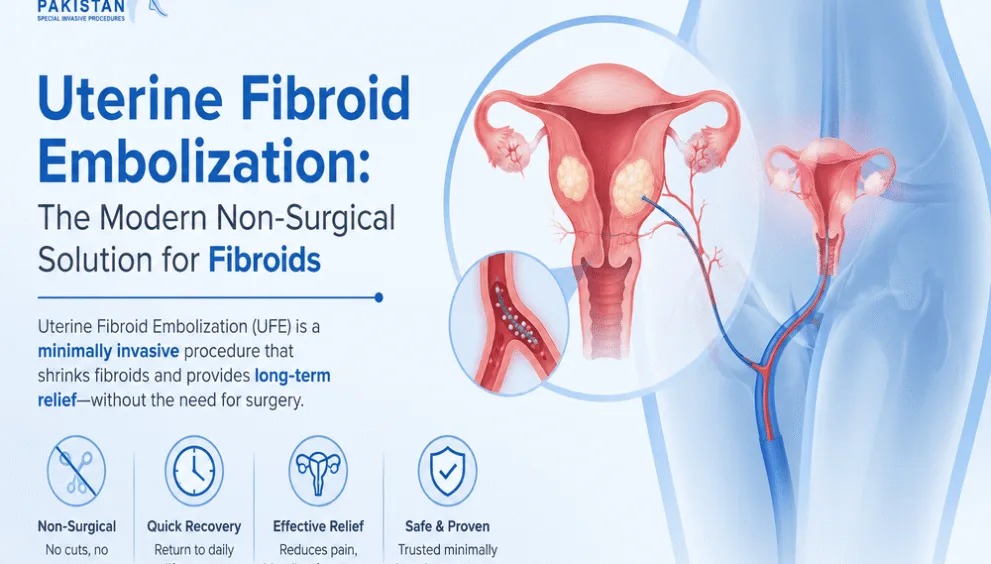
Uterine Fibroid Embolization: The Modern Non-Surgical Solution for Fibroids
Breaking Free from Fibroid Symptoms
For decades, women suffering from uterine fibroids have faced a painful dilemma: endure debilitating symptoms or undergo major surgery. Heavy menstrual bleeding that requires changing protection every hour, severe pelvic pain that interrupts daily life, and the constant worry about fertility have forced countless women to choose between their quality of life and their reproductive health.
But what if there was a third option?
Uterine Fibroid Embolization (UFE) has revolutionized how women manage fibroids in Pakistan and globally. This minimally invasive procedure offers relief from fibroid symptoms without the recovery time, surgical risks, or fertility concerns associated with traditional hysterectomy or myomectomy.
According to recent studies, over 80% of women experience significant symptom improvement after UFE, with many returning to normal activities within 2 weeks.
If you’re struggling with uterine fibroids and want to understand your treatment options, this comprehensive guide explores everything you need to know about UFE—from how it works to recovery timelines and cost considerations.
What are Uterine Fibroids? Understanding the Condition
What are Uterine Fibroids?
Uterine fibroids, also called leiomyomas, are benign (non-cancerous) growths that develop in or around the uterus. They are composed of smooth muscle and connective tissue and vary significantly in size—from microscopic nodules to masses larger than a grapefruit.
Key Facts About Fibroids:
- Prevalence: Affect 70-80% of women by age 50
- Malignancy Risk: Less than 0.1% ever become cancerous
- Symptom Severity: Highly variable—some women have no symptoms, while others experience debilitating effects
- Multiple Development: Women often develop multiple fibroids simultaneously
Common Fibroid Types:
Submucosal Fibroids (Project into uterine cavity)
- Cause heavy menstrual bleeding
- Most likely to affect fertility
- Most responsive to treatment
Intramural Fibroids (Embedded in uterine wall)
- Most common type (60% of cases)
- Cause pain and pressure
- May affect fertility depending on size
Subserosal Fibroids (Protrude from uterus exterior)
- Often don’t cause menstrual symptoms
- May cause pressure/pain on surrounding organs
- Rarely affect fertility
Symptoms of Uterine Fibroids: When to Seek Treatment
Not all fibroids cause symptoms. However, when symptoms occur, they significantly impact quality of life:
Primary Symptoms:
- Heavy Menstrual Bleeding: Periods lasting 7+ days, sometimes with clots
- Pelvic Pain & Pressure: Discomfort in lower abdomen, pelvis, or lower back
- Frequent Urination: Fibroids pressing on bladder
- Bowel Dysfunction: Constipation or diarrhea from intestinal compression
- Pain During Intercourse: Dyspareunia from fibroid location
- Infertility Issues: Difficulty conceiving or recurrent miscarriage
Secondary Consequences:
- Anemia: From chronic heavy bleeding (iron deficiency)
- Fatigue: Result of anemia and chronic pain
- Emotional Distress: Impact on mental health and relationships
- Reduced Fertility: Depends on fibroid location and size
Traditional Fibroid Treatment Options: Why They Fall Short
Traditional Treatments for Uterine Fibroids
Before exploring UFE, it’s important to understand why women often seek alternatives to conventional treatments:
Medical Management (Medication)
Hormonal Birth Control
- Effectiveness: Reduces bleeding 30-50%
- Limitations: Doesn’t shrink fibroids; temporary solution
- Timeline: Continuous use required
- Cost: PKR 2,000-5,000/month
GnRH Agonists (Lupron, Zoladex)
- Effectiveness: Shrinks fibroids 40-60%
- Limitations: Side effects mimic menopause (hot flashes, bone loss), temporary effect
- Timeline: Max 6 months; fibroids regrow after stopping
- Cost: PKR 15,000-25,000/injection (monthly)
Progestin IUD (Mirena)
- Effectiveness: Reduces bleeding 80%
- Limitations: Doesn’t shrink fibroids; displacement risk
- Timeline: 5-year device lifespan
- Cost: PKR 40,000-60,000 initial
Surgical Options
Myomectomy (Fibroid Removal)
- Recovery: 4-6 weeks
- Risks: Scarring, anesthesia complications, recurrence (10-30% within 5 years)
- Fertility: Preserved but may affect pregnancy
- Cost: PKR 300,000-500,000
- Limitations: Multiple surgeries often needed; fibroids often recur
Hysterectomy (Uterus Removal)
- Recovery: 6-8 weeks
- Risks: Major surgery risks, loss of fertility, early menopause symptoms
- Fertility: Permanently eliminated
- Cost: PKR 400,000-700,000
- Permanence: Guaranteed fibroid relief but permanent
- Psychological Impact: Significant for women wanting future pregnancies
Limitations of Traditional Approaches:
- Medical therapy is temporary and doesn’t address root cause
- Surgery carries anesthesia and complications risks
- Hysterectomy eliminates fertility permanently
- Myomectomy has high recurrence rates
- Long recovery times affect work and daily life
What is Uterine Fibroid Embolization (UFE)?
Uterine Fibroid Embolization represents a paradigm shift in fibroid management. Unlike surgery that removes fibroids or the uterus, UFE works by cutting off the blood supply to fibroids, causing them to shrink naturally.
How UFE Works:
The Procedure in Simple Terms:
Imagine fibroids as tumors that need constant blood flow to survive. By blocking the arteries supplying these fibroids, we starve them of oxygen and nutrients, causing them to gradually die and shrink.
Step-by-Step Process:
- Vascular Access (5 minutes)
- Local anesthesia applied to groin
- Catheter (thin tube) inserted into femoral artery
- Patient remains conscious (conscious sedation provided)
- Diagnostic Angiography (10 minutes)
- Contrast dye injected to visualize uterine arteries
- Confirms fibroid location and vascularity
- Identifies arterial branches supplying fibroids
- Selective Catheterization (15 minutes)
- Catheter advanced into right uterine artery
- Positioned precisely at fibroid-feeding arteries
- Continuous fluoroscopic imaging guides placement
- Embolization – Right Side (10 minutes)
- Embolic material (polyvinyl alcohol particles or spheres) injected
- Particles lodge in arteries, blocking blood flow
- Angiography confirms complete arterial blockade
- Contralateral Embolization (10 minutes)
- Catheter withdrawn and repositioned in left uterine artery
- Same embolization process repeated on left side
- Bilateral embolization achieves maximum fibroid shrinkage
- Final Angiography & Completion (5 minutes)
- Confirms bilateral arterial occlusion
- Verifies no off-target embolization
- Catheter removed; hemostasis achieved
Total Procedure Time: 45-90 minutes
What Material is Used for Embolization?
Polyvinyl Alcohol (PVA) Particles
- Most common material
- Particle size: 300-500 microns
- Biodegradable nature allows some recanalization
- Cost-effective
Embospheres (Calibrated Microspheres)
- More uniform size distribution
- More predictable arterial occlusion
- Reduced off-target embolization
- Preferred in experienced centers
- Premium cost
Tris-acryl Gelatin Microspheres
- Biocompatible synthetic material
- Longer-lasting occlusion
- Fewer retreatment rates
- Growing preference in modern centers
Why Uterine Fibroid Embolization? Key Advantages
UFE has transformed fibroid management due to its remarkable advantages over traditional approaches:
1. Minimally Invasive Approach
- No surgical incisions (only needle puncture)
- No general anesthesia required
- Conscious sedation provides comfort without intubation
- Perfect for anxious patients
- No scarring or tissue trauma
2. Rapid Recovery
- Same-day discharge (most cases)
- 1-2 weeks to normal activities (vs. 4-6 weeks for surgery)
- No work restrictions within days
- Minimal pain (NSAIDs usually sufficient)
- No lengthy hospital stays
3. Fertility Preservation
- Uterus remains intact (unlike hysterectomy)
- Ovarian function preserved (unlike surgical removal)
- Natural pregnancy possible (30-40% conception rate within 12 months)
- No impact on hormone production
- Better outcomes than myomectomy in many studies
4. Superior Symptom Relief
- 80-90% experience significant improvement
- Heavy bleeding reduction: 90%+ of patients
- Pelvic pain relief: 70-80% within 3-6 months
- Pressure symptoms: Typically resolve within weeks
- Symptom improvement timeline: 3-6 months (compared to years with medication)
5. Comprehensive Fibroid Treatment
- Treats all fibroids simultaneously (myomectomy addresses only surgically accessible ones)
- Multiple fibroids managed in single procedure
- Prevents new fibroid development from nutrient deprivation
- Addresses both symptomatic and asymptomatic fibroids
6. Cost-Effectiveness
- UFE Cost in Pakistan: PKR 200,000-400,000 (varies by center)
- Myomectomy Cost: PKR 300,000-500,000
- Hysterectomy Cost: PKR 400,000-700,000
- Lower cost + faster recovery = better overall value
- Insurance coverage increasingly available
7. No General Anesthesia Risks
- Eliminates anesthesia-related complications
- Suitable for patients with medical comorbidities
- No surgical airway management needed
- Lower infection risk vs. surgery
- Suitable for older patients
8. Durable Long-Term Results
- Symptom recurrence: Only 10-15% at 5 years
- Hysterectomy rate post-UFE: <5% (vs. 30%+ after myomectomy)
- Long-term satisfaction: >85% at 5-year follow-up
- Effects last years, not months like medication
UFE Compared to Other Treatments: A Comprehensive Comparison
| Factor | UFE | Myomectomy | Hysterectomy | Medical Therapy |
|---|---|---|---|---|
| Invasiveness | Minimally invasive | Surgical | Surgical | Non-invasive |
| Anesthesia | Conscious sedation | General | General | None |
| Hospital Stay | Same-day | 1-3 days | 2-4 days | Outpatient |
| Recovery Time | 1-2 weeks | 4-6 weeks | 6-8 weeks | Ongoing |
| Fertility | Preserved | Preserved | Eliminated | Preserved |
| Symptom Relief | 80-90% | 80-90% | 100% | 30-50% |
| Recurrence Rate | 10-15% | 20-30% | 0% | High (stops use) |
| Repeated Treatment | Possible | Possible | N/A | Continuous |
| Cost | PKR 200-400K | PKR 300-500K | PKR 400-700K | PKR 2-25K/month |
| Pain/Downtime | Minimal | Moderate-Severe | Moderate-Severe | None |
| Scar Tissue | None | Possible | None | None |
| Sexual Function | Preserved | Preserved | Variable | Preserved |
| Uterus Preserved | Yes | Yes | No | Yes |
Bottom Line: UFE offers the best balance of symptom relief, fertility preservation, minimal downtime, and reasonable cost.
The UFE Procedure: What to Expect
Before the Procedure:
Pre-Procedure Evaluation (1-2 weeks before)
- Imaging studies: MRI or pelvic ultrasound to assess fibroid characteristics
- Blood tests: Verify kidney function (for contrast dye) and coagulation
- Medical clearance: Physician evaluation ensures candidacy
- Medication review: Some medications adjusted or paused
- Discussion: Review procedure details, risks, and expectations with radiologist
Preparation Day:
- NPO (Nothing by mouth) for 6 hours before procedure
- Light breakfast allowed 6 hours prior if early afternoon procedure
- Remove jewelry and metallic objects
- Wear comfortable, loose clothing
- Arrange transportation (sedation requires driver)
- Light activity recommended evening before
During the Procedure:
Expected Timeline:
- Arrival: 90 minutes before procedure (registration, IV placement)
- Preparation: 20 minutes (positioning, sterile draping, local anesthesia)
- Procedure: 45-90 minutes (actual embolization)
- Recovery: 1-2 hours (post-anesthesia monitoring)
- Discharge: After vital sign stabilization and pain control
Patient Experience:
- Local anesthesia felt as brief stinging sensation
- Conscious sedation provides relaxation (patients often sleep through procedure)
- Catheter insertion felt as pressure sensation
- No pain during embolization (fibroids have no pain receptors)
- Post-embolization discomfort managed with IV pain medication
- Continuous monitoring via pulse oximetry, blood pressure, heart rate
Important Note: While the procedure itself is minimally painful, post-embolization syndrome (cramping, pain) is common and expected as fibroids begin necrosis.
After the Procedure:
Immediate Post-Procedure (0-2 hours)
- Continuous monitoring in recovery area
- IV pain medication and antiemetics as needed
- Bed rest for groin hemostasis (prevents bleeding)
- Hydration with IV fluids
- Discharge criteria: Stable vital signs, pain controlled, ambulating independently
First 24-48 Hours (Post-Embolization Syndrome)
- Expected: Pelvic cramping, vaginal discharge, low-grade fever
- Management: Oral analgesics, anti-inflammatory medication
- Duration: 24-72 hours typically (rarely extends beyond 1 week)
- Severity: Varies from mild discomfort to moderate cramping
- Red Flags: Fever >101.5°F, severe pain, heavy vaginal bleeding—contact physician
First Week:
- Return to light activities as tolerated
- Avoid heavy lifting, strenuous exercise, sexual activity
- Pain typically improves significantly by day 3-4
- Vaginal discharge (brownish/bloody) normal for 2-4 weeks
- Most women return to work by day 7-10
2-6 Weeks:
- Progressive return to normal activities
- Exercise gradually increased (walking → moderate activity)
- Sexual activity typically resumed by week 3-4
- Work schedule normalized
- Residual symptoms (spotting) resolve
3-6 Months:
- Maximum symptom improvement occurring
- Heavy bleeding typically reduced 90%+
- Pelvic pain significantly diminished
- Energy levels returning as anemia improves
- Fibroids shrinking progressively on imaging
UFE Success Rates: Real-World Outcomes
Clinical evidence demonstrates UFE’s remarkable effectiveness:
Symptom Improvement Rates:
Heavy Menstrual Bleeding
- Complete resolution: 40-50%
- Significant reduction (>75%): 85-90%
- Failure rate: <5%
- Timeline: Maximum improvement by 6 months
Pelvic Pain & Pressure
- Complete resolution: 50-60%
- Significant improvement: 75-80%
- Failure rate: <5%
- Timeline: Progressive improvement over 3-6 months
Infertility (Pre-Procedure)
- Conception achieved: 30-40% within 12 months post-UFE
- Higher in younger patients and those with previously preserved ovarian reserve
- Myomectomy comparison: Similar conception rates, but myomectomy has scar tissue complications
- Note: UFE doesn’t reverse pre-existing infertility factors
Long-Term Durability:
Five-Year Outcomes:
- Symptom recurrence: 10-15%
- Hysterectomy rate post-UFE: <5% (vs. 30% after myomectomy)
- Re-embolization needed: 5-10%
- Patient satisfaction: >85%
- Quality of life improvement: Sustained across study period
Ten-Year Data (Limited but Growing):
- Symptom control: 70-75% remain satisfied
- Hysterectomy rate: 5-10%
- Demonstrates long-term efficacy
- Aging effects on results continue to be studied
Comparison to Myomectomy (Surgery):
Why UFE Has Better Long-Term Outcomes Than Myomectomy:
- Treats ALL fibroids (surgery addresses only visible ones)
- No scar tissue formation (surgery creates adhesions)
- Lower recurrence rate (new fibroids less likely)
- No repeat surgery needed (myomectomy recurrence rate 10-30%)
- Lower hysterectomy rate post-UFE vs post-myomectomy
UFE Risks & Complications: Being Transparent
Like any medical procedure, UFE carries potential risks. However, serious complications are rare when performed by experienced interventional radiologists.
Common Side Effects (Expected, Temporary):
Post-Embolization Syndrome (Most frequent)
- Frequency: 60-80% of patients
- Symptoms: Pelvic cramping, vaginal discharge, low-grade fever, malaise
- Duration: 24-72 hours typically (rarely >1 week)
- Severity: Mild to moderate
- Management: NSAIDs, analgesics, rest
- Outcome: Resolves completely without intervention
Minor Vaginal Discharge
- Frequency: 40-60%
- Appearance: Brownish, bloody, or foul-smelling
- Duration: 2-4 weeks post-UFE
- Cause: Fibroid necrosis, endometrial sloughing
- Management: Observation, pads (not tampons)
- When concerned: Foul odor + fever suggests infection
Menstrual Cycle Changes
- Frequency: 20-30% temporary changes
- Types: Longer cycles, irregular periods, spotting
- Duration: Usually 3-6 months normalization
- Cause: Endometrial regeneration after necrosis
- Outcome: Most restore normal cycling
Moderate Complications (Infrequent):
Fibroid Expulsion (Passage of necrotic fibroid tissue)
- Frequency: 5-15% (higher with submucosal fibroids)
- Presentation: Vaginal passage of tissue, severe cramping
- Management: Usually spontaneous; occasionally needs D&C
- Timeline: Typically occurs 4-12 weeks post-UFE
- Outcome: Usually beneficial as fibroid is expelled
Infection/Sepsis
- Frequency: 1-2% (higher with large fibroids)
- Presentation: Fever >101.5°F, severe pain, elevated WBC
- Cause: Infected necrotic fibroid tissue
- Management: IV antibiotics; rarely needs hospital admission
- Prevention: Prophylactic antibiotics during procedure
Non-Target Embolization
- Frequency: <1% with experienced operators
- Risk: Ovarian vessels, bladder vessels accidentally embolized
- Prevention: Selective catheterization, careful angiographic assessment
- Outcome: May affect ovarian function or bladder function if occurs
Rare Serious Complications (<1%):
Arterial Dissection
- Catheter-related vascular injury
- Risk: <0.5%
- Prevention: Careful catheter manipulation, proper training
- Management: Stent placement if significant
Contrast-Induced Nephropathy
- Kidney dysfunction from contrast dye
- Risk: <1% (higher in renal disease patients)
- Prevention: Adequate hydration, renal-protective medications
- Monitoring: Creatinine levels post-procedure
Uterine Necrosis
- Full thickness uterine ischemia (extremely rare)
- Risk: <0.1%
- Prevention: Careful bilateral embolization technique
- Outcome: Would require hysterectomy (but essentially never occurs)
Premature Ovarian Failure
- Loss of ovarian function post-UFE
- Risk: Rare but documented; <1% documented cases
- Variables: Age >45, large fibroids, extensive collateral flow
- Monitoring: FSH levels if amenorrhea occurs
Risk Factors for Complications:
Higher Risk Patients:
- Age >50 (larger fibroids, more fragile vasculature)
- Large fibroid burden (>500g total fibroid mass)
- Renal disease (contrast sensitivity)
- Diabetes (delayed healing)
- Heavy smokers (vascular disease)
- Prior uterine surgery (scar tissue)
UFE Success Factors: Who Benefits Most?
Ideal Candidates for UFE: ✓ Women with symptomatic fibroids (bleeding, pain, pressure) ✓ Multiple fibroids (better for UFE than surgery) ✓ Desire fertility preservation ✓ Want to avoid hysterectomy ✓ Prefer minimal downtime recovery ✓ Medical comorbidities making surgery risky ✓ Age 30-55 (sweet spot for outcomes) ✓ Normal renal function (for contrast use)
Relative Contraindications: ✗ Active infection (uterine, pelvic) ✗ Severe renal disease (contrast contraindicated) ✗ Iodine allergy (contrast allergy) ✗ Uncorrected coagulopathy (bleeding risk) ✗ Pregnancy (obvious) ✗ Only desire is fertility (other options may be better)
Special Considerations:
Women Planning Pregnancy:
- UFE is safe and doesn’t prevent pregnancy
- Higher success with younger age (<35 years)
- Miscarriage rates: Similar to general population
- Premature delivery: Slightly increased (2-3%) but small absolute increase
- Recommendation: Attempt pregnancy for 6-12 months post-UFE before considering alternative
Adolescents with Fibroids:
- Unusual presentation (typically older women)
- UFE may be performed; preserves future fertility
- Growing evidence supports safety in younger women
- Long-term data still accumulating
Women Approaching Menopause:
- Good candidates if symptomatic
- Shorter duration of symptom relief needed
- Lower risk of future pregnancy concerns
- Consider individual symptoms vs. near-future menopause
UFE vs. Focused Ultrasound Surgery (MRgFUS)
Alternative Minimally Invasive Option:
Magnetic Resonance-guided Focused Ultrasound Surgery uses focused ultrasound waves to ablate fibroids while monitoring via MRI.
Comparison:
| Factor | UFE | MRgFUS |
|---|---|---|
| Procedure Time | 45-90 min | 1-4 hours |
| Invasiveness | Catheter-based | Non-invasive |
| Anesthesia | Conscious sedation | General anesthesia |
| Recovery | 1-2 weeks | 1-2 weeks |
| All Fibroids Treated | Yes | Selective (not all) |
| Symptom Relief Rate | 80-90% | 60-75% |
| Fertility Impact | Preserved | Preserved |
| Cost | PKR 200-400K | PKR 400-600K (not widely available in Pakistan) |
| Availability in Pakistan | Available | Limited/Unavailable |
Conclusion: UFE remains superior for comprehensive fibroid treatment, especially in Pakistani context where MRgFUS unavailable.
UFE in Pakistan: What You Need to Know
Availability & Centers:
IRCC Pakistan (Interventional Radiology & Vascular Treatment Center)
- Location: D.H.A. Lahore; clinics in Karachi, Islamabad
- Dr. Shahbaz Ahmed Qazi: Foreign-trained Interventional Radiologist
- Experience: 25+ years; 250,000+ successful procedures
- Specialization: Highest UFE volume in Pakistan
- Expertise: 100% patient satisfaction (UFE outcomes)
Cost in Pakistan:
UFE Pricing Range:
- Standard UFE: PKR 200,000-300,000
- Complex cases (large fibroids, multiple): PKR 300,000-400,000
- Insurance: Increasingly covered by major health insurers
- Payment Plans: Some centers offer installment options
Pre-Procedure Arrangements in Pakistan:
Required Investigations:
- Pelvic ultrasound or MRI (confirm diagnosis, assess fibroid characteristics)
- Complete blood count, coagulation profile
- Renal function tests (creatinine, BUN)
- Pregnancy test (exclude pregnancy)
- Medical clearance if >50 years old
Timeline:
- Consultation: 1-2 weeks scheduling
- Investigations: 3-5 days after consultation
- Procedure scheduling: Usually 1-2 weeks after imaging
Practical Considerations:
- Arrange 24-hour companion for post-procedure care
- Take 3-5 days off work minimum
- Plan transportation (cannot drive after sedation)
- Keep follow-up appointment at 1 month
Recovery Timeline: What to Expect Week by Week
Immediate (0-24 hours)
- Post-anesthesia grogginess (4-6 hours)
- Pelvic cramping (manageable with pain medication)
- Mild nausea possible (IV antiemetics given)
- Monitor groin puncture site (no bleeding should occur)
- Bed rest for first 4-6 hours post-procedure
Week 1
- Days 1-3: Most intense cramping (post-embolization syndrome)
- Pain Management: Ibuprofen, acetaminophen, prescribed analgesics
- Activity: Light walking encouraged; avoid lifting >5 kg
- Work: Consider working from home if desk job
- Vaginal Discharge: Expect brownish/bloody discharge
- Fever: Low-grade fever common (manageable with NSAIDs)
Week 2
- Cramping diminishes significantly
- Pain mostly resolved (occasional discomfort)
- Return to normal daily activities
- Light exercise (walking, stretching) okay
- Most patients back to work
- Vaginal discharge continuing (normal)
Weeks 3-4
- Minimal pain
- Resume normal exercise gradually
- Sexual activity usually safe to resume
- Discharge may continue but decreasing
- Feel much improved overall
- Follow-up imaging scheduled (optional month 1)
Weeks 5-8
- Essentially back to normal
- Modest exercise (jogging, gym) typically safe
- Heavy strength training still avoided
- Discharge nearly resolved
- Energy returning as anemia improves
- Symptom improvement becoming apparent
Months 2-3
- Complete return to normal activities
- All restrictions lifted
- Significant symptom improvement expected
- Heavy bleeding typically resolved
- Pelvic pain substantially improved
- Follow-up imaging at 3-month mark (shows fibroid shrinkage)
Months 3-6
- Maximum symptom improvement reached
- Fibroids continue shrinking on imaging
- Full return to exercise, sports
- All post-procedure effects resolved
- Begin attempting pregnancy if desired
- Significant quality of life improvement
Frequently Asked Questions About UFE
Fertility & Pregnancy
Q1: Can I get pregnant after UFE?
Yes. Natural pregnancy is possible in 30-40% of women attempting pregnancy within 12 months post-UFE. Success depends on:
- Age (younger = better outcomes)
- Other infertility factors
- Fibroid characteristics
- Ovarian reserve
Important note: UFE doesn’t improve infertility from other causes (low sperm count, ovulation disorders), but removes the fibroid barrier to conception.
Q2: Is miscarriage rate increased after UFE?
Miscarriage rates post-UFE are similar to general population (15-25%) at same maternal age. Some studies suggest very slight increase (2-3%), but risk remains low.
Q3: How long should I wait to try conceiving after UFE?
Most experts recommend waiting 3-6 months post-UFE to allow:
- Complete endometrial healing
- Fibroid involution stabilization
- Full physical recovery
However, pregnancy occurring before 3 months is not contraindicated; outcomes similar to later pregnancies.
Q4: Are there complications for pregnancy after UFE?
Potential pregnancy complications (though uncommon):
- Placental abnormalities (rare but documented)
- Intrauterine growth restriction (very rare)
- Preterm labor (slight increase 2-3%)
- Cesarean delivery rate (higher than general population)
Overall: Vast majority of UFE patients have uncomplicated pregnancies and deliveries.
Recovery & Activity
Q5: How long until I can return to work?
- Desk job: 3-7 days
- Physical job: 2-4 weeks
- Heavy labor: 4-6 weeks
- Most common: 1-2 weeks before full return
Q6: When can I resume exercise?
- Walking: Immediately (encourage within 24 hours)
- Light cardio: Week 2-3
- Moderate exercise: Week 4-5
- Heavy strength training: Week 6+
- Full unrestricted exercise: Month 2-3
Q7: When is sexual activity safe?
- Recommendation: After vaginal discharge stops (usually 2-4 weeks)
- Most authorities suggest 2-3 weeks minimum
- Start gently; pain should be absent before resumption
- Contraception not immediately needed (pregnancy unlikely first 3 months)
Risks & Complications
Q8: What’s the risk of needing hysterectomy after UFE?
Risk of hysterectomy post-UFE is <5% at 5 years, compared to:
- 30%+ after myomectomy (symptom recurrence)
- 0% after initial hysterectomy (obviously)
Hysterectomy typically pursued only if:
- Severe infection developing (very rare)
- Symptoms completely unrelieved
- Patient changes mind about fertility
Q9: Will UFE cause premature menopause?
Premature ovarian failure (early menopause) post-UFE is extremely rare (<1%).
Risk factors if present:
- Age >45
- Large fibroid burden
- Extensive collateral ovarian circulation
Monitoring: FSH levels checked if amenorrhea develops post-UFE.
Q10: Is there radiation exposure with UFE?
Yes, minimal. Fluoroscopy during procedure delivers:
- Effective dose: 2-5 millisieverts (mSv)
- Equivalent to: 5-15 years natural background radiation
- Cancer risk increase: Negligible (estimated <1:1000)
- Compared to: One CT scan = 7-10 mSv
For perspective: Risk from living in brick house = more radiation than single UFE procedure.
Cost & Insurance
Q11: What’s included in UFE cost?
Typical package includes:
- Procedure (interventional radiologist, equipment, embolic material)
- Conscious sedation/anesthesia
- Post-operative pain management
- Hospital facility
- Post-op monitoring
- Follow-up ultrasound or imaging
NOT included:
- Pre-procedure investigations (ultrasound, blood work)
- Hospital admission if needed (rare)
- Complications management if arise
Q12: Is UFE covered by insurance?
Coverage varies:
- PMDC (Pakistan): Increasingly approved
- Private insurers: Many now cover (check policy)
- SECP-regulated: Most cover after pre-authorization
- Military/Government: Usually covered
- International insurance: Often covered
Recommendation: Pre-authorization check before procedure.
Q13: Are payment plans available?
Many centers offer:
- Installment plans (3-6 months interest-free)
- Negotiable rates for self-pay patients
- Corporate partnerships for employee discounts
- Special schemes for retired individuals
Specific Fibroid Situations
Q14: Can UFE treat all fibroid types?
Yes, UFE treats:
- Submucosal fibroids ✓
- Intramural fibroids ✓
- Subserosal fibroids ✓
- Multiple fibroids ✓
- Large fibroids (>15 cm) ✓
However, outcomes vary:
- Submucosal: Highest success rate (90%+)
- Intramural: Excellent (85-90%)
- Subserosal: Good if causing symptoms (70-80%)
Q15: What if I have very large fibroids?
UFE works for large fibroids (up to 15+ cm), but:
- Procedure may take longer
- Post-embolization syndrome may be more intense
- Fibroid expulsion more common (5-15%)
- Shrinkage takes longer (6-12 months vs. 3-6 months)
- May need D&C if expelled fibroid causes issues
Still preferred to surgery in most cases.
Q16: Can UFE prevent future fibroids from developing?
UFE doesn’t prevent new fibroid development, but:
- Recurrence rate lower than after myomectomy (10-15% vs. 20-30%)
- Why: Embolized vessels may not regenerate to same extent
- Why lower than surgery: No surgical trauma = less vascular disruption
Essentially: UFE reduces, but doesn’t eliminate, fibroid recurrence risk.
Real Patient Success Stories
Case 1: Sarah, Age 32 – Infertility Concern
Chief Complaint: Heavy periods, pelvic pain, unable to conceive for 2 years
Imaging: Large intramural fibroid (8 cm), no other infertility factors identified
Treatment: UFE with successful bilateral uterine artery embolization
Timeline:
- Month 1 post-UFE: Periods much lighter; cramping resolved
- Month 3: Imaging shows 50% fibroid shrinkage
- Month 6: Fibroid shrunk to 3 cm; normal menstrual cycle restored
- Month 8: Positive pregnancy test
Outcome: Successful delivery of healthy 3.2 kg baby at 38 weeks (scheduled vaginal delivery)
Patient Quote: “I went from desperate for surgery to avoiding it entirely. The UFE changed everything.”
Case 2 : Fatima, Age 45 – Excessive Bleeding
Chief Complaint: Severe menorrhagia (changing pads every 1-2 hours), profound anemia (Hgb 7.2), declining quality of life
Imaging: Multiple intramural and subserosal fibroids (total burden 450g)
Prior Treatment: Failed hormonal therapy (GnRH agonists caused menopausal symptoms)
Treatment: UFE despite large fibroid burden; procedure took 90 minutes
Timeline:
- Days 1-3: Moderate cramping (controlled with ibuprofen)
- Week 1: Period stopped (amenorrhea); dramatic relief
- Month 1: Hemoglobin 9.8 (improving); no heavy bleeding
- Month 3: Hemoglobin 11.2 (normal range); normal light periods
- Month 6: Sustained normal periods; fibroids shrunk 60%; feel like “new person”
Outcome: Avoided hysterectomy; returned to hiking, activities she’d abandoned; hemoglobin normalized
Patient Quote: “I had written off anything but hysterectomy. Getting my life back was incredible.”
Case 3: Aisha, Age 49 – Pressure Symptoms
Chief Complaint: Constant pelvic pressure, frequent urination (8+ times/night), lower back pain; bleeding mild but lifestyle severely restricted
Imaging: Massive subserosal fibroid (12 cm) causing bladder/bowel compression
Surgical Consideration: Surgeon recommended hysterectomy (size/symptoms); patient declined
Treatment: UFE; catheter positioning carefully navigated despite fibroid vasculature complexity
Timeline:
- Week 1: Urinary frequency improving
- Week 4: Nighttime voiding reduced to 1-2 times
- Month 2: Pressure sensation resolved; back pain gone
- Month 4: Imaging shows 40% shrinkage
- Month 6: Fibroid shrunk to 7 cm; asymptomatic; normal quality of life
Outcome: Avoided major surgery; resumed normal activities; avoided hysterectomy’s long-term hormonal effects
Patient Quote: “Being able to sleep through the night again… that alone was worth it.”
When to Consider UFE: A Decision-Making Framework
Choose UFE When:
✓ You have symptomatic fibroids that impact quality of life ✓ You want to avoid surgery but need symptom relief ✓ Fertility is a concern (want to preserve reproductive potential) ✓ You have multiple fibroids (better than repeated surgeries) ✓ You want rapid recovery and minimal downtime ✓ You’re not ready for hysterectomy even if recommended ✓ Medical comorbidities make surgery risky (diabetes, heart disease, obesity) ✓ You’ve failed medical management (hormonal therapy inadequate) ✓ You want comprehensive treatment of all fibroids simultaneously
Consider Alternatives When:
- Primary goal is fertility and fibroids are small → Myomectomy may be preferred
- Fibroids are small/asymptomatic → Observation is appropriate
- You’re unwilling to accept any fibroid recurrence risk → Hysterectomy is only true cure
- You have MRgFUS availability and prefer non-invasive option → Explore this alternative
- Severe renal disease → Contrast contraindicated (though alternative approaches exist)
- You absolutely decline any risk → Medical therapy (imperfect but zero procedural risk)
NOT Recommended When:
- Currently pregnant
- Active intrauterine infection
- Uncorrected coagulopathy
- Contrast allergy (iodine) without alternative imaging
- Unwilling to accept <1% small complication risk
Expert Recommendations & Guidelines
Professional Society Position Statements:
American College of Radiologists (ACR): “UFE is established as safe and effective for symptomatic uterine fibroids, particularly for women wanting to preserve fertility or avoid surgery.”
Society of Interventional Radiology (SIR): “UFE represents a first-line minimally invasive option for women with symptomatic fibroids seeking symptom relief with fertility preservation.”
American College of Obstetricians & Gynecologists (ACOG): “UFE is an acceptable alternative to surgery or medical management for appropriate candidates with symptomatic fibroids.”
European Society of Human Reproduction & Embryology (ESHRE): “UFE does not preclude future pregnancy; women should be counseled about potential for improved fertility post-UFE.”
Key Takeaways: Why UFE is Pakistan’s Premier Fibroid Solution
- Minimally Invasive: No surgical incisions, conscious sedation, same-day discharge
- Effective: 80-90% symptom improvement; treats all fibroids simultaneously
- Fertility-Preserving: Uterus intact; natural pregnancy possible; 30-40% conception rate
- Fast Recovery: 1-2 weeks vs. 4-8 weeks for surgery
- Durable: Long-term results; only 10-15% symptom recurrence at 5 years
- Safe: Complication rates <2%; serious complications <1%
- Cost-Effective: PKR 200-400K; comparable to surgery with better outcomes
- Pakistan Access: Available at IRCC and major centers nationwide
- Established: 30+ years evidence base; millions performed globally
- Expert Available: Dr. Shahbaz Qazi brings international expertise to Pakistani patients
Taking the Next Step: How to Pursue UFE
Step 1: Consultation
- Schedule initial consultation with interventional radiologist
- Discuss symptoms, fertility goals, treatment preferences
- Physician assesses candidacy based on clinical presentation
Step 2: Imaging Assessment
- Pelvic ultrasound or MRI for precise fibroid characterization
- Determines fibroid number, size, location, vascularity
- Critical for procedural planning
Step 3: Pre-Procedure Workup
- Blood tests: CBC, coagulation, renal function
- Pregnancy test: Rule out pregnancy
- Medical clearance: If age >50 or significant comorbidities
- Education: Discussion of procedure, risks, recovery
Step 4: Procedure Scheduling
- Confirm date convenient to patient
- Arrange transportation and care companion
- Finalize pre-procedure instructions
- Insurance pre-authorization if applicable
Step 5: Procedure Day
- Arrive 90 minutes early
- Light anesthesia, minimal anxiety
- 45-90 minute procedure
- 1-2 hour recovery; discharge with care instructions
Step 6: Recovery & Follow-Up
- Week 1: Manage post-embolization syndrome
- Month 1: Follow-up imaging optional
- Month 3: Imaging confirms fibroid shrinkage
- Month 6: Full symptom improvement assessment
Step 7: Long-Term Monitoring
- Annual pelvic exams
- Imaging only if symptoms recur
- Pregnancy monitoring if attempting conception
- Reassurance and education ongoing
Contact Information for IRCC Pakistan UFE Services
IRCC Pakistan (Interventional Radiology & Cardiovascular Center)
Main Office: 153/1, F Block, Phase 5, D.H.A., Lahore, Pakistan +92-332-4520052 | +92-331-0232883 | +92-334-0005020 irccpakistan@gmail.com , www.irccpakistan.com
Dr. Shahbaz Ahmed Qazi
- Foreign-trained Interventional Radiologist
- 25+ years experience
- 250,000+ successful procedures
- Specialized expertise in UFE
Available At Multiple Locations:
- Lahore (Main facility)
- Karachi
- Islamabad
Conclusion: Reclaiming Your Life from Fibroids
Uterine fibroids have stolen enough from you—your comfort, your confidence, your peace of mind. For too long, women accepted limited choices: medication that didn’t work, surgery with lengthy recovery, or hysterectomy that ended reproductive potential.
UFE changes this equation entirely.
With 80-90% of women experiencing significant symptom improvement, minimal downtime, fertility preservation, and long-lasting results, Uterine Fibroid Embolization represents the modern answer to an ancient problem.
Whether you’re struggling with heavy bleeding that interferes with work, pelvic pain that limits activities, or fertility challenges from fibroids, UFE offers hope. You don’t have to accept fibroids as a permanent part of your life.
The evidence is clear. The outcomes are proven. The choice is yours.
Take the first step today. Schedule your UFE consultation with IRCC Pakistan and discover how you can reclaim your health, your fertility, and your life.